UC San Diego study links blood biomarker p-tau217 to women’s dementia risk up to 25 years ahead
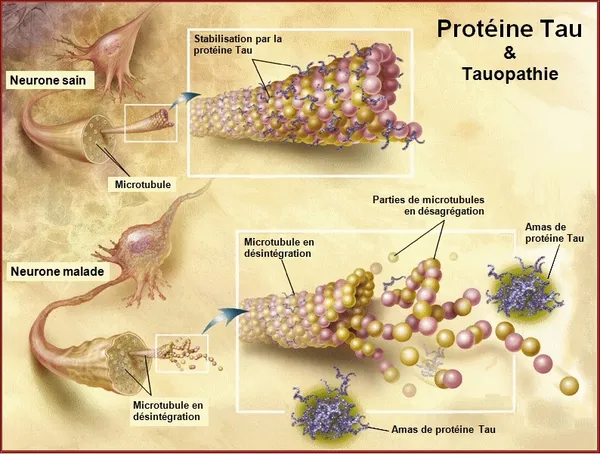
A long-term cohort study examines whether a tau-related blood marker can flag future cognitive decline
Scientists affiliated with the University of California San Diego report that a blood-based biomarker associated with Alzheimer’s disease pathology was strongly linked to later development of mild cognitive impairment and dementia in older women, with follow-up extending as long as 25 years.
The research analyzed baseline blood samples from women who were cognitively unimpaired at enrollment and then tracked clinical outcomes over subsequent decades. The biomarker measured was phosphorylated tau at threonine 217 (p-tau217), a tau protein form tied to neurodegenerative changes seen in Alzheimer’s disease.
Study design and population
The analysis drew on 2,766 participants enrolled in the Women’s Health Initiative Memory Study. Participants were ages 65 to 79 when recruited in the late 1990s and were followed for up to 25 years. Blood samples collected at the start of the study were later tested for p-tau217, and participants were monitored for onset of mild cognitive impairment and dementia.
Investigators evaluated whether baseline p-tau217 levels predicted future clinical outcomes and assessed whether associations differed across subgroups, including by age at baseline, genetic risk, race, and hormone therapy assignment.
Key findings reported
- Higher baseline p-tau217 levels were associated with increased risk of developing mild cognitive impairment and dementia during follow-up.
- Associations with dementia were reported to be stronger among women older than 70 at baseline compared with those younger than 70.
- Stronger associations were also reported among women with the APOE ε4 genetic risk factor for Alzheimer’s disease.
- Relationships between p-tau217 and dementia outcomes varied by hormone therapy assignment: the association was reported to be stronger among women randomized to estrogen plus progestin compared with placebo, while differences were not reported in the same way for estrogen alone versus placebo.
- Predictive performance using p-tau217 together with age was reported to be similar in White and Black women, though some differences by race were also described in subgroup analyses.
The researchers said the long interval between baseline testing and later clinical outcomes suggests blood-based biomarkers could help identify elevated dementia risk years before symptoms emerge.
What the findings do and do not mean for patients
The study focuses on prediction of future risk in women who had no measurable cognitive impairment at baseline. It does not establish that p-tau217 causes dementia, and it does not demonstrate that identifying elevated p-tau217 decades earlier leads to improved health outcomes.
The researchers noted that blood-based biomarkers are not currently recommended for routine clinical use in people without cognitive symptoms. Further studies are needed to determine how such testing could be used in everyday care, including how results should be interpreted alongside age, genetics, and health factors, and what interventions—if any—should follow an elevated result.
Why the result is being watched closely
Blood-based biomarkers are of interest because they may be less invasive and more scalable than brain imaging or cerebrospinal fluid testing. This study’s long follow-up period and focus on women adds to evidence that blood markers tied to Alzheimer’s biology may help stratify risk well before clinical diagnosis, while also highlighting that predictive strength can differ across clinical and demographic subgroups.